What is Cervical Cancer?
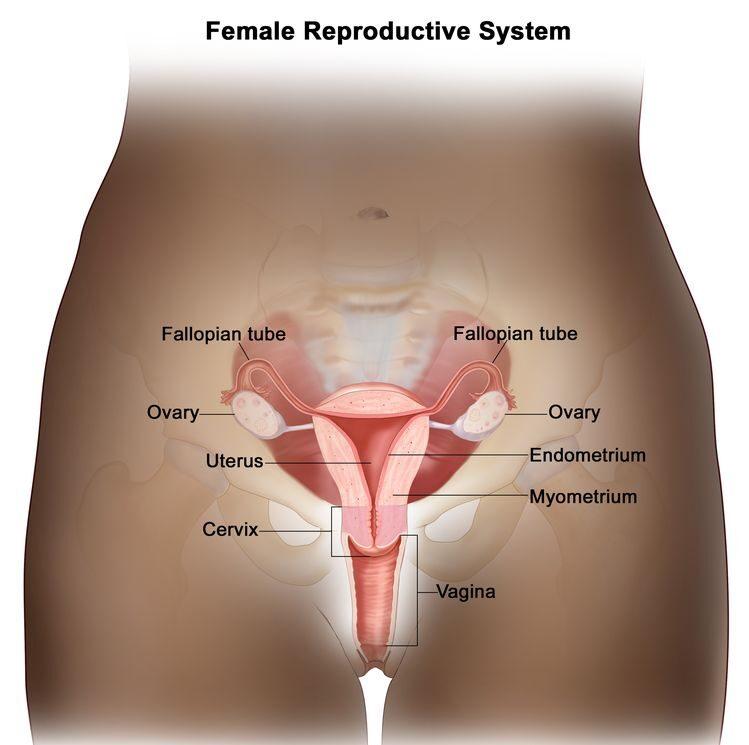
Cervical cancer is cancer that starts in the cells of the cervix. The cervix is the lower, narrow end of the uterus (womb). The cervix connects the uterus to the vagina (birth canal). Cervical cancer usually develops slowly over time. Before cancer appears in the cervix, the cells of the cervix go through changes known as dysplasia, in which abnormal cells begin to appear in the cervical tissue. Over time, if not destroyed or removed, the abnormal cells may become cancer cells and start to grow and spread more deeply into the cervix and to surrounding areas.
The cervix has two main parts:
- The ectocervix (also called exocervix) is the outer part of the cervix that can be seen during a gynecologic exam. The ectocervix is covered with thin, flat cells called squamous cells.
- The endocervix is the inner part of the cervix that forms a canal that connects the vagina to the uterus. The endocervix is covered with column-shaped glandular cells that make mucus.
The squamocolumnar junction (also called the transformation zone) is the border where the endocervix and ectocervix meet. Most cervical cancers begin in this area.
Types of cervical cancer
Cervical cancers are named after the type of cell where the cancer started. The two main types are:
- Squamous cell carcinoma: Most cervical cancers (up to 90%) are squamous cell carcinomas. These cancers develop from cells in the ectocervix.
- Adenocarcinoma: Cervical adenocarcinomas develop in the glandular cells of the endocervix. Clear cell adenocarcinoma, also called clear cell carcinoma or mesonephroma, is a rare type of cervical adenocarcinoma.
Sometimes, cervical cancer has features of both squamous cell carcinoma and adenocarcinoma. This is called mixed carcinoma or adenosquamous carcinoma. Very rarely, cancer develops in other cells in the cervix.
Cervical Cancer Symptoms
Early on, cervical cancer usually doesn’t have symptoms, making it hard to detect. Symptoms usually begin after the cancer has spread.
When symptoms of early-stage cervical cancer do occur, they may include
- vaginal bleeding after sex
- vaginal bleeding after menopause
- vaginal bleeding between periods or periods that are heavier or longer than normal
- vaginal discharge that is watery and has a strong odor or that contains blood
- pelvic pain or pain during sex
Symptoms of advanced cervical cancer (cancer has spread beyond the cervix to other parts of the body) may include the symptoms of early-stage cervical cancer and
- difficult or painful bowel movements or bleeding from the rectum when having a bowel movement
- difficult or painful urination or blood in the urine
- dull backache
- swelling of the legs
- pain in the abdomen
- feeling tired
These symptoms may be caused by many conditions other than cervical cancer. The only way to know is to see a health professional. If it is cervical cancer, ignoring symptoms can delay treatment and make it less effective.
Cervical Cancer Causes, Risk Factors, and Prevention
HPV infection causes cervical cancer
Long-lasting (persistent) infection with high-risk types of human papillomavirus (HPV) causes virtually all cervical cancers. Two high-risk types, HPV 16 and HPV 18, cause 70% of cervical cancers worldwide.
Nearly all people who are sexually active will become infected with HPV at some point in their lives. Most HPV infections go away on their own within a year or two as the immune system controls the infection. These short-term infections do not cause cancer. When a high-risk HPV infection lasts for years, it can lead to changes in the cervical cells, resulting in a precancerous lesion. If the precancerous lesion is not found and removed, it may eventually develop into cervical cancer.
People who become sexually active at a young age, especially before age 18, or have multiple sexual partners are more likely to become infected with a high-risk type of HPV.
Factors that increase the risk that an HPV infection will cause cancer
Some risk factors make it more likely for a person who has a high-risk HPV infection of the cervix to develop cervical cancer. These risk factors include:
- Having a weakened immune system. This can lower the body’s ability to fight an HPV infection. HPV infections are more likely to be persistent and progress to cancer in people who are immunocompromised than in people who are not immunocompromised. You may be immunocompromised if you:
- have an HIV infection or another disease that weakens your immune system
- take medicine to suppress your immune response, such as to prevent organ rejection after a transplant, to treat an autoimmune disease, or to treat cancer
- Smoking or breathing in secondhand smoke. People who smoke or breathe in secondhand smoke have an increased risk of developing cervical cancer. The risk increases the more a person smokes or is exposed to secondhand smoke.
Learn about different tools to help you quit smoking and how to use them.
- Reproductive factors. Both the use of oral contraceptives (birth control pills) and giving birth to many children are associated with an increased risk of cervical cancer. The reasons for these associations are not well understood.
- Obesity. Cervical cancer screening may be more difficult in those with obesity, leading to lower detection of precancers and a higher risk of cancer.
DES exposure is a rare cause of cervical cancer
Being exposed to a drug called diethylstilbestrol (DES) in the womb is an independent risk factor for a type of cervical cancer called clear cell adenocarcinoma. Between 1940 and 1971, DES was given to some pregnant women in the United States to prevent miscarriage (premature birth of a fetus that cannot survive) and early labor. Women whose mothers took DES while pregnant have an increased risk of cervical cell abnormalities and of clear cell adenocarcinoma of the vagina and cervix.
Cervical cancer is preventable
Cervical cancer is highly preventable and highly curable if caught early. Nearly all cervical cancers could be prevented by HPV vaccination, routine cervical cancer screening, and appropriate follow-up treatment when needed.
HPV vaccination
HPV vaccination is a safe and effective way to help prevent cervical cancer. Gardasil 9 is the FDA-approved vaccine for females and males aged 9 to 45 in the United States. Gardasil 9 is approved to prevent precancers and cancers caused by seven cancer-causing HPV types (16, 18, 31, 33, 45, 52, and 58) and to prevent genital warts caused by HPV types 6 and 11. The HPV vaccine does not treat an existing HPV infection.
Timing of HPV vaccination
The HPV vaccine offers the most protection when given before a person becomes sexually active. Those who are already sexually active may benefit less from the vaccine. This is because sexually active people may have been exposed to some of the HPV types the vaccine targets.
The Centers for Disease Control and Prevention (CDC) recommends routine HPV vaccination for girls and boys at age 11 or 12, and the vaccine can be given starting at age 9. For young people who weren’t vaccinated within the age recommendations, HPV vaccination is recommended up to age 26. Some adults between the ages of 27 and 45 who are not already vaccinated may decide to get the HPV vaccine after talking with their doctor about their risk of new HPV infections.
The HPV vaccine is given as a series of two or three doses, depending on age. CDC recommends that children who start the vaccine series before age 15 receive two doses. For people who receive the first dose on or after their 15th birthday, and for people with certain immunocompromising conditions, CDC recommends getting three doses.
Cervical cancer screening
Because HPV vaccination doesn’t protect against all HPV types that can cause cervical cancer, getting screened at regular intervals is still important.
Two widely used screening tests are HPV tests and cytology tests (also known as Pap test or Pap smear). These tests can find high-risk HPV infections and abnormal cell changes and precancers that can be treated before they turn into cancer. So it is important for people with a cervix to have regular screening tests starting in their 20s.
For cervical cancer screening to be effective, people need to get timely screening and follow up of abnormal test results. Because of social, environmental, and economic disadvantages, certain groups may have difficulty accessing health care and, as a result, bear a disproportionate burden of cervical cancer.
Condoms
Condoms, which prevent some sexually transmitted diseases, can decrease the risk of HPV transmission. However, they do not completely prevent it. Therefore, exposure to HPV is still possible in areas that are not covered by the condom.

